Liver Transplantation
Dr. Nikhil Shellagi
MS Surgery, DNB Surgical Gastroenterology Fellowship in HPB and Liver Transplantation

Best Liver Transplant Surgeon in Bangalore
Liver Surgery
In general, liver surgery is required in kids and adults who are suffering from constant liver dysfunction because of various reasons and where the benefits of transplantation out weight the risk of alternative modalities.
The most usual indications for liver transplantation are hepatitis b and c infection and alcoholic liver disease. Liver transplantation is a life-saving system for patients with chronic end-stage liver disease and selected patients with acute liver failure. Meanwhile, if know about what is Gallbladder Surgery.
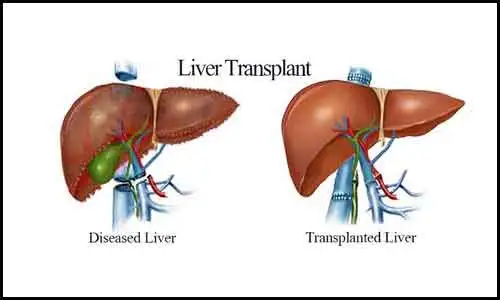
1) Cirrhosis including:
- Alcohol related cirrhosis
- Biliary cirrhosis (primary or secondary)
- Chronic active hepatitis (A, B, C, non A, non B, autoimmune)
- Congenital biliary cirrhosis
- Cryptogenic cirrhosis
- Hemochromatosis
- Alpha I Antitrypsin Deficiency
- NASH
2) Extrahepatic biliary atresia
3) Fulminant hepatic failure
4) Inherent errors of metabolism including
- Alpha-I antitrypsin
- Crigler-Najjar disease, Type I
- Byler’s disease
- Glycogen storage disease, Type I
- Wilson’s disease
- Hemochromatosis
- Tyrosinemia
- Wolman’s disease
- Familial amyloidotic polyneuropathy
- Primary hyperoxaluria type 1
5) Primary Sclerosing cholangitis
6) Hepatocellular Carcinoma (HCC), Stage I or II, or: single lesion
Living Donor Liver Transplant
In a living-donor liver transplant, a portion of a healthy living person’s liver is surgically removed and implanted into the abdomen of a patient whose liver is no longer functioning normally.
Within a few months of the operation, the donor’s remaining liver grows and regains its normal size, volume, and capacity. At the same time, the recipient’s transplanted liver portion develops and returns to normal liver function.
Benefits of a liver transplant from a living donor
This type of surgery offers several important advantages because it utilises a portion of a liver from a living donor rather than a liver from a deceased donor:
- Shorter Waits: Usually, living donors are a recipient’s family member or close family. This implies that there is no need to wait on a list.
- Faster Recovery: Patients who receive organs from living donors recover more quickly and are less likely to need dialysis or blood transfusions after surgery.
- Better Results: Compared to recipients of deceased donor livers, recipients of living donor livers have an average 5-per cent higher long-term survival rate.
What transpires during liver transplant surgery using living donors?
The removal of the donor liver and subsequent implanting into the recipient typically take four to six hours each for a living donor liver transplant.
To access the liver, the surgeon will first make a lengthy incision across the donor’s abdomen.
(A smaller laparoscopic incision will be made if the patient is a child.)
The remainder of the liver that has been determined to be sufficient for the recipient will then be removed.
The liver may contain this region in amounts ranging from 25 to 65 per cent. They will stop the bleeding, close the wound, and take the donor to the hospital for treatment.
The surgeons will implant the donor-recipient with the healthy liver portion in the second stage of the procedure. As they did for the donor, they will first make a lengthy incision across the recipient’s abdomen.
The existing liver will then be removed after its connections have been severed. The implant of the donor liver portion will come last.
To do this, the donor liver will be connected to the patient’s veins, arteries, and bile ducts.
The donor liver will be able to function normally and important connections will be restored as a result. The surgeon will then finish by closing the incision.
Once implanted, the liver will immediately start to regenerate itself in both the donor and recipient. Typically, this procedure takes six to eight weeks to complete.
The following are some steps in the evaluation process:
- Blood tests: Determine your blood’s compatibility with the recipient’s blood as well as the health of your thyroid, liver, and kidneys. Additionally tests for communicable diseases like HIV and hepatitis.
- Physical Examination: A doctor will examine you if your blood types are compatible to ascertain your general state of health.
- Magnetic Resonance Imaging (MRI): Gives doctors a precise image of your internal organs so they have a surgical “road map” to follow.
- CECT Abdomen (Triphasic) Screening tests: These may include an exercise stress test, an echocardiogram (EKG), and a pulmonary function test as needed.
- Additional Consultations: You will also meet with a psychiatrist to discuss the donation process with you and to evaluate your mental health.
How long will it take the liver donor to recover completely?
Most donors typically reach full recovery after three to six weeks. The time needed for recovery varies depending on the donor.
Donors will visit the hospital regularly during this time to track their recovery. The hospital staff will help each donor determine when they can resume regular activities and return to work by carefully evaluating their health.
Data from lab tests, observations of any signs or symptoms, and assessments made by the patient and staff all contribute to this choice.
What is the survival rate for recipients of living donors?
The Organ Procurement and Transplantation Network (OPTN) data showed that between 2008 and 2015, the national survival rate for living donor transplants was:
Within a year of surgery, 92% three years after surgery, 88% five years after surgery, 84%
Comparatively, the survival rates for transplants from deceased donors during the same time were:
91% percent a year after surgery Three years after surgery, 83% 75% five years after surgery
These figures represent the average survival rate for people of all ages, including the very young and old and the critically ill.
Even higher survival rates are anticipated for patients between the ages of 1 and 65 with less severe liver diseases.
Deceased Donor Liver Transplant
When a patient does not have a family member, loved one or other individual willing and able to donate a liver, a transplant from a deceased donor is the only option.
What Does a Deceased Donor Liver Transplant Involve?
Deceased donor livers come from people who have died suddenly, usually from an accident or bleed into the brain. These individuals are usually between one and 70 years of age and have been relatively healthy before their death.
These people have previously expressed to their families a willingness to donate their organs, or their families have made the decision to donate their organs so that someone else will have a chance to live a better life.
It isn’t necessary to match the donor and recipient for age, sex or race. All donors are screened for hepatitis viruses and the HIV virus.
What’s more, all deceased donor organs are tested extensively to help ensure that they don’t pose a health threat to the recipient. Also, many studies – such as ABO blood type and HLA matching – are performed to ensure that the organs are functioning properly.
As soon as a deceased donor is declared brain-dead, the liver is removed and placed in sterile fluid similar to fluid in body cells. It is then stored in the refrigerator.
The harvested liver needs to be transplanted within 12 hours of recovery – which is why recipients are often called to the hospital in the middle of the night or at short notice.

