Hepatobiliary and Pancreatic Surgery
Dr. Nikhil Shellagi
MS Surgery, DNB Surgical Gastroenterology Fellowship in HPB and Liver Transplantation

Hepatobiliary and Pancreatic Surgery in Bangalore
Hepatobiliary Surgery and Pancreatic Surgery
Liver Hydatid cyst, large hemangioma, Biliary cystadenoma, Hepatocellular carcinpma.Intra hepatic cholangiocarcinoma, Surgery for colorectal, neuroendocrine liver metastasis, Major liver rescetion for advanced gall bladder cancer and hilar cholangiocarcinoma
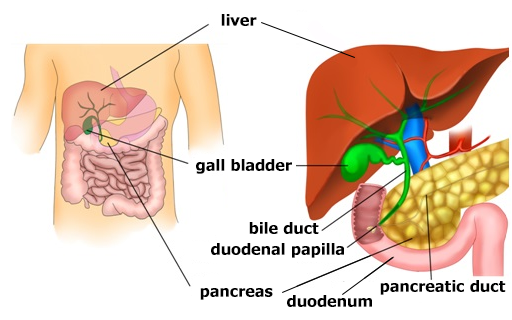
- Bile Duct stones, surgery for benign biliary strictures, cholangiocarcinoma
- Gallbladder stones, gall bladder cancer
- Pancreas: Minimal Invasive Pancreatic Necrosectomy, Surgery for Chronic Pancreatitis, cystic tumours of pancreas, whipple’s procedure for pancreatic head cancer, Distal apncreatectomy for pancreatic body and tail tumours
- Spleen: Surgery for large splenic cyst, splenic abscess, splenic tumours Shunt surgery ; Proximal and distal splenorenal shunt, mesocaval shunt
Chronic Pancreatitist Here
Chronic pancreatitis (CP) is a benign pancreatic inflammatory process characterized by progressive and irreversible organ damage that eventually results in pain, exocrine and endocrine insufficiency, malnutrition, and/or other symptoms.
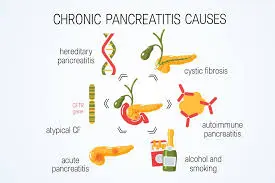
- Toxic-metabolic (alcohol/tobacco)
- Idiopathic
- Genetic (Trypsinogen gene mutations)
- Autoimmune
- Recurrent and severe acute pancreatitis
- Obstructive (divisum or tumor)
Pain: Abdominal pain is the most common and morbid symptom occurring in the majority of patients (90%) and is responsible for most hospital admissions related to CP. The pain is located in the epigastric area, often radiates to the back, is dull or boring in quality and worsens after eating
Endocrine insufficiency (diabetes mellitus): Endocrine insufficiency also occurs late in the disease. It is reported to the tune of 20–30% in various Indian studies. It can be controlled with diet, OHAs and insulin therapy.
Exocrine insufficiency: Pancreatic exocrine insufficiency may be mild, moderate or severe depending on the stage of the disease process, duration of disease and aetiology.
Typically, fatty diarrhoea (steatorrhea) does not become clinically apparent until 90 per cent of pancreatic function has been lost.

Various complications include pseudocysts, biliary or duodenal obstruction, internal or external pancreatic fistulae, left-sided portal hypertension and pancreatic malignancy.
Biochemical measurements:
Patients with chronic pancreatitis may have low, normal, or elevated levels of isoamylase, lipase, trypsin, and elastase.
It can be challenging to make a firm diagnosis of chronic pancreatitis in early or mild cases based solely on serum enzyme levels.
Radiological Examination:
Plain Abdominal Film: The plain abdominal film is typically the initial diagnostic procedure used to confirm the presence of chronic pancreatitis. As a positive finding, diffuse, specked calcification of the gland might be sufficient.
Trans abdominal ultrasound is a straightforward, non-invasive, and reasonably priced imaging method.
Large cavities (greater than 1 cm), calcification, and a dilated pancreatic duct (greater than 4 mm) are all signs of chronic pancreatitis (70 per cent sensitivity and 90 per cent specificity).
The following are the crucial components of managing a CP patient:
(1) Reduction of discomfort;
(2) Uphold nutrition and manage malnutrition
(3) Address complications.
Control of abdominal pain: The aim of therapy is to keep the patient’s pain under control, as complete pain relief is not anticipated.
The following techniques are employed to reduce the discomfort:
Analgesics: antioxidant enzymes in the pancreas.
Pregabalin Nerve Blocks: The two nerve block techniques used to prevent pancreatic pain afferents from signalling to the spinal cord are celiac plexus blockade (CPB) and celiac plexus neurolysis (CPN).
Endoscopic Therapy: The goal of endotherapy is to reduce ductal hypertension and relieve PD outflow obstruction in order to relieve pain.
Liver Cancer
Liver cancer is a disorder that occurs in the liver. The liver is the biggest glandular organ in the body and plays many important roles to keep the body clear of viruses and dangerous substances.
In adults, renal cell carcinoma is the most usual type of liver cancer — about 90 % of cancerous tumors. A few general kinds of liver cancer can occur. Growing children are more likely to develop a kind of liver cancer called Wilms’ tumor.
Hepatocellular carcinoma
The hepatocytes, the main liver cells, are affected by this condition. It can spread from the liver to various body regions, including the abdomen, intestines, and pancreas.
Cholangiocarcinoma
The short, tube-like bile ducts in the liver are where cholangiocarcinoma, more commonly known as bile duct cancer, starts. Bile is transported through these tubes to the gallbladder to aid in digestion.
Liver Angiosarcoma
A rare form of liver cancer called liver angiosarcoma develops in the liver’s blood vessels. Due to the rapid growth of this type of cancer, it is frequently discovered at a more advanced stage.
Hepatoblastoma
Hepatoblastoma is a very rare type of liver cancer. It’s nearly always seen in kids, especially those under age 3. With surgery and chemotherapy, the risk for people with this kind of cancer can be really good.
Factors that can raise the risk of liver cancer include:
Older age
Your risk of liver cancer rises as you age.
Smoking
Smokers have a higher risk of liver cancer than nonsmokers do. The risk reduces after you quit.
Obesity
People who are overweight have a higher risk of liver cancer than people who are held normal weight.
High blood pressure (hypertension)
High blood pressure raises your risk of liver cancer
- Dropping weight without working
- Lack of appetite
- Upper gastric pain
- Illness and vomiting
- General debility and fatigue
- Abdominal swelling
- Yellow stain of your skin and the whites of your eyes
- White, gray stools
Blood Investigations
Tumour Markers: AFP
USG Abdomen
CECT Abdomen
MR Abdomen
PETCT
Surgery
The following procedures are used to treat liver cancer:
1 . Surgery to remove the tumour: If the tumour is small and the liver is healthy, doctors who specialise in liver cancer may perform operations to remove the tumour and some healthy liver tissues.
Surgery to replace the diseased liver with a healthy liver from a donor is known as liver transplantation.
Liver transplant surgery: In a liver transplant, the diseased liver is replaced with a healthy liver from a donor.
2 . Radiation treatment: If all other treatments fail, radiation therapy is used. It also controls the signs and symptoms of cancer.
Radiation therapy uses powerful energy from sources like protons and X-rays to kill cancer cells and shrink tumours. The energy is carefully directed toward the liver while the surrounding healthy tissue is spared.
The patient is said to lie on a table during an external beam radiation therapy treatment while a beam is allowed to pass at a specific location on their body.
3. Targeted drug therapy
Targeted drug therapy focuses on certain abnormalities present within cancer cells. By killing these abnormalities through targeted drug cancer cells are allowed to die.
4. Immunotherapy
Immunotherapy uses an internal immune system of a patient to fight with cancer. Sometimes the immune system of a patient is unable to attack cancer as the cancer cells produce proteins that blind the immune system cells. Immunotherapy is used to improve this process. It is used for patients with advanced liver cancer.
5. Chemotherapy
Chemotherapy employs drugs to kill cancer cells that are dividing quickly. You can take pills to treat it, inject them into a vein in your arm, or do both.
Bile Duct
Rare tumours with a poor prognosis are bile duct neoplasms. The bile duct is a tiny, 10 to 15 centimeter-long tube that connects the liver and gallbladder to the small intestine to transport bile. Here, bile aids in the digestion of dietary fat. Any area of the bile duct can become the site of bile duct cancer.
Adenocarcinoma, also known as cholangiocarcinona, is the most prevalent type of bile duct cancer and occurs when cancer cells grow in the mucus glands (a group of cells that produce fluid) that line the interior of the bile duct.
Based on where cancer has spread, bile duct cancer is divided into three groups:
- Cancers of the intrahepatic bile duct (within the liver)
- Cancers of the perihilar bile duct (ducts leaving the liver)
- Cancer of the distal bile duct (ducts closer to the small intestine)
- Jaundice (yellow skin)
- Body itchiness spread throughout
- Dark yellow urine or light-colored stools
- stomach ache
- Loss of appetite or weight
- nausea or diarrhoea
- Fever
Normally procedures for hepatobiliary tumours include:
Ultrasonography,
Digital Tomography (CT)
Imaging Using Magnetic Resonance (MRI)
Endosonography, cholangiography (endoscopic or percutaneous), Positron Emission Tomography (PET), cholescintigraphy, and angiography are additional techniques.
The following serum tumour markers have been linked to bile duct carcinomas:
cancer-causing antigen (CEA)
CA 19-9, a carbohydrate antigen.
The latter has an 80 percent specificity and a 75 percent sensitivity for values over 100 U/mL.
Treatment can be curative (with intent to cure, aiming for long term survival) or palliative (aiming to prolong survival and/or improve life quality and postpone disease symptoms).
The only standard curative option is the complete surgical resection.
Unfortunately, most patients (nearly 90% according to some authors) are not candidates for curative treatment. It is usually for unresectable advanced/metastatic tumour. Some patients are not capable of radical surgery due to their performance status. In these and other cases that sadly form the majority of clinical situations, palliative care is the option.
The procedure for hilar cholangiocarcinoma typically involves an extended right hepatectomy as well as a right or left trisegmentectomy, which is associated with a high rate of perioperative mortality (0 percent to 19 percent ). This is in part because major hepatic resection carries a higher risk of postoperative liver failure.
Since Makuuchi et al. first suggested portal vein embolization for hilar cholangiocarcinoma, it has gained widespread acceptance as a helpful preoperative measure in the event of extensive liver resection with a subsequent small liver remnant volume.
Selectively occluding the main portal branch to the liver parenchyma that will be removed causes compensatory hypertrophy of the remaining liver parenchyma, which typically increases by 8 to 20 percent over the course of 2 to 6 weeks.
In general, patients who need a future liver remnant volume of less than 25% to 35% of the original liver volume may benefit from portal vein embolization.
Pancreaticoduodenectomy (Whipple’s PD): The standard procedure of choice for the complete removal of distal bile duct cancer is pancreaticoduodenectomy (Whipple’s PD), in conjunction with porta hepatis lymphadenectomy.
Extended hepatectomy for hilar cholangiocarcinoma: Extended right- or left-hemihepatectomy is regarded as the standard radical operation for hilar cholangiocarcinoma based on the mode of tumour extension, the radicality, and the ease of the procedure.
Liver transplantation for hilar cholangiocarcinoma: Liver transplantation for hilar cholangiocarcinoma: Orthotopic liver transplantation (OLT) may provide the benefit of complete resection of all tumor-involved structures, including vessels within the hepatoduodenal ligament, all intra- and extrahepatic bile ducts, and the entire liver parenchyma, for the treatment of locally advanced hilar cholangiocarcinoma beyond the indication for resection.
Prognostic Factors are:
- Lymph node involvement
- The extent of the resection
- Tumor differentiation
These have an impact on the patient’s long-term survival.
Pancreatic Cancer

Exocrine tumors: This form of pancreatic cancer is the most prevalent. The most fundamental variety of exocrine tumors is adenocarcinoma. Ductal adenocarcinomas, the term for these tumor cells, typically begin in the pancreatic tubes. Acinar adenocarcinoma is the name for the tumor that develops in the acini.
The diagnosis of intraductal papillary mucinous neoplasm is one that is frequently made (IPMN). An IPMN is a tumor that develops inside the pancreas’ ducts and produces mucin, a solid fluid. If IPMN is not treated promptly, it may eventually develop into cancer. When an IPMN is operated on, it occasionally already has progressed to cancer.
Acinar cell carcinoma, adenosquamous carcinoma, colloid carcinoma, giant cell tumor, hepatoid carcinoma, mucinous cystic neoplasms, pancreatoblastoma, serous cystadenoma, signet ring cell carcinoma, solid and pseudopapillary tumor, squamous cell carcinoma, and undifferentiated carcinoma are some uncommon types of exocrine pancreatic tumors.
Endocrine tumors: These are also referred to as islet cell tumors or pancreatic neuroendocrine tumors (PNETs). They differ from exocrine tumours in this regard. A pancreatic neuroendocrine tumor only occasionally functions. Only a tumor in active growth produces hormones. The hormone produced by cells serves to define a neuroendocrine tumor.
They include: Insulinoma, Gastrinoma, Glucagonoma, Somatostatinoma, VIPomas, PPomas.
- Age (risk of developing pancreatic cancer increases with age)
- Gender (More females are affected rather than males)
- Drinking and Smoking (access amount may be the cause of pancreatic cancer an early age)
- Diet and obesity (being overweight)
- Diabetes
- Family history (it accounts for less than 10% of cases)
- families with two or more first-degree relatives who have pancreatic cancer (parent, brother, sister, or child)
- families with three or more members on the same side of the family suffering from pancreatic cancer
- families where at least one member has pancreatic cancer and there is a family cancer syndrome. Rare genetic conditions known as family cancer syndromes increase the risk of pancreatic cancer due to a defective gene.
- uncommon inherited illnesses.
- processed and red meat
- surgery for the gall bladder and gallstones
The majority of the time, pancreatic cancer symptoms appear after the disease progresses.
Pancreatic cancer symptoms could include:
- Jaundice (yellow eyes, Light-colored or greasy stools,
- Dark urine, itchy skin)
- Belly (abdomen) ache or backache
- loss of weight and reduced appetite (bloating)
- nausea and vomiting and diarrhea
- liver or gallbladder enlargement
- Clots of blood
- Diabetes
Typically, these symptoms do not indicate pancreatic cancer.
However, if you see any of them for longer than two weeks, see a doctor.
Imaging tests: These examinations help your doctors see your internal glands, including the pancreas, by taking pictures of your internal organs. Ultrasound, computerised tomography (CT) scans, magnetic resonance imaging (MRI), and, occasionally, positron emission tomography (PET) scans are used to diagnose pancreatic cancer.
Ultrasound: (Using a scope to create pictures of your pancreas) An ultrasound scanner is used during an endoscopic ultrasound (EUS) to take images of your pancreas from inside your abdomen. To obtain the images, the instrument is passed down your oesophagus and into your stomach using an endoscope, which is a small, flexible tube.
Chemotherapy Systemic Chemotherapy: Drugs are used to stop the division or death of cancer cells in order to stop the spread of the disease.
Chemotherapy enters the bloodstream when taken orally or administered intravenously or intramuscularly, where it can reach cancer cells all over the body.
Regional chemotherapy: The cerebrospinal fluid, an organ, or a body cavity, such as the abdomen, are injected directly with drugs that primarily target the cancer cells in those regions.
Combination Chemotherapy: The use of multiple anticancer medications. The type and stage of the cancer being treated determine how the chemotherapy is administered.
Radiation Treatment: To kill cancer cells or stop them from proliferating, it uses high-energy x-rays or other forms of radiation. Two types of radiation therapy exist:
Radiation therapy is applied externally. Radiation is directed toward cancer by a machine outside the body.
Internal radiation therapy: is the use of radioactive material that has been sealed inside of needles, seeds, wires, or catheters and is inserted into or close to cancer.
The two differ depending on the kind and stage of the cancer being treated. Recovery from Surgery The majority of patients who undergo surgery for pancreatic cancer recover without any issues. These people return home in two to four days.
Fewer patients might recover more slowly and require a little longer of a wait. You will receive instructions from a surgeon on how to care for yourself, including advice on bathing, driving, and sexual activity.
Information about you will be provided:
- Diet
- Exercise
- Pain medicine
- Bowel movements
Diet Exercise Painkillers
Pelvic motions
You’ll receive a Daily Goals Checklist after treatment. Utilize that checklist to gauge your progress each day.
Expertise in treating pancreatic cancer belongs to Dr. Nikhil Shellagi. He provides options for chemotherapy and targeted therapy in addition to the best surgical treatment for pancreatic cancer.
Gall Bladder Cancer
Gallbladder cancer (GBC) is a rare but notoriously deadly cancer that exhibits significant racial and geographic variations. The northern and northeastern Indian states of Uttar Pradesh, Bihar, Orissa, West Bengal, and Assam have the highest rates of GBC.
In northern India, it is the most prevalent digestive cancer in women and affects them twice as frequently as men. Along with gallstones, other risk factors for the development of GBC include female gender, ethnicity, genetic susceptibility, and lifestyle choices.

